William H. Calvin and George A. Ojemann, Inside the Brain: Mapping the Cortex, Exploring the Neuron (New American Library, 1980), chapter 3. See also http://WilliamCalvin.com/Bk1/bk1ch3.htm. |
William H. Calvin
University of Washington |

|
3
Reading, Writing, and Speaking: Where Does Language Live? |
©1980 by William H. Calvin and George A. Ojemann |
The rapid voltage fluctuations characteristic of a "resting" epileptic focus are seen all along Neil's left temporal lobe, much as the earlier scalp EEG had suggested. However, they are seen far enough in the rear of the temporal lobe to cause the neurosurgeon some concern, as this area and the adjoining parietal lobe are very important for language. just as one does not remove the cells which control movement, one does not remove language portions of the brain to control seizures: the cure would be worse than the disease. But what are the boundaries of the language part of Neil's brain? Do they overlap the epileptic focus, or is there a strip in between of healthy but nonlanguage brain tissue? "Well, Neil, so far, so good. Now we'll set up the slide show for you. Everything okay?" asks the neurosurgeon. "Oh, I'm fine. And if it's the same slide show as before, it's about the easiest test that I've ever taken."
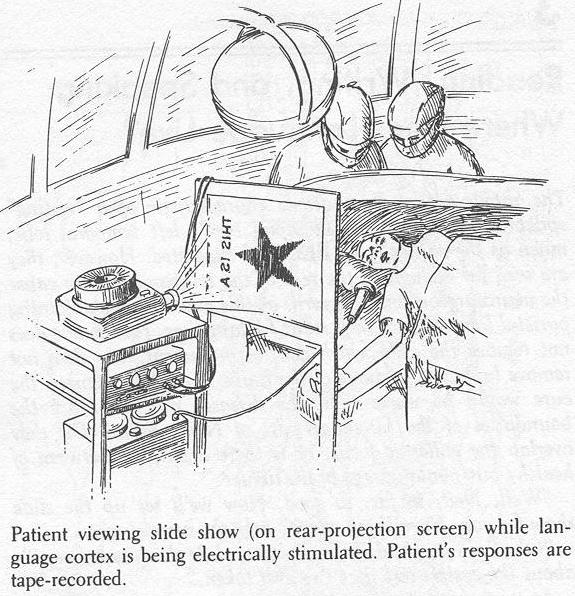
Neil, who had been resting quietly, listening to everyone discuss his EEG interpretation, is now put to work again. The night before, Neil was trained on a simple test of Ian guage and memory. The apparatus for it is now set up in the OR. There is a slide projector and a small projection screen. The slides are shown sideways on the screen so that Neil, lying on his side, sees them normally. Everyone else in the OR can be seen lilting their heads sideways to watch. The first slide is a sketch of a star. Neil says, "This is a star. " The next slide is just the number 84. Neil knows that his task is to count backward by threes, so he begins "84, 81, 78, 75 ..." The third slide just has the word "Recall" on it. Neil stops counting and replies "Star." 
The fourth slide is a sketch of a house, so Neil says, "This is a house." Another number comes up, and he again counts backward by threes to distract him from rehearsing the name that he will need to recall six seconds later. Over and over the three-slide sequence repeats, using sketches of many different common objects. This series of tasks is hardly difficult, particularly with the previous night's practice, and Neil would ordinarily make few mistakes. But during the surgery, electrical stimulation is applied to the brain during certain Parts of the sequence, not applied during others. The electrical stimulation is weak enough that Neil cannot tell when it occurs. Unlike the stimulation of motor strip, stimulation of speech and language areas does not evoke speech; rather, it confuses things so that a small area of cortex does not function properly.
"This is . . . it's a . you know, it's a . . . I just can't . . ." Neil can talk, but he cannot find the right name for the object. Interestingly enough, after the electrical stimulation is turned off and Neil has counted backward by threes and the "recall" slide has appeared, he may now be able to recall the correct name. This test of naming helps to identify the language areas of the brain for the neurosurgeon. The neurosurgeon moves the silver stimulating wires around over the exposed surface of the brain during the test, keeping track of the spots where the stimulation disrupts naming by laying another little numbered paper tag on the spot. Sometimes, the electrical stimulation is given while Neil is counting backward by threes, just after Neil has correctly named the sketch of the object. Neil continues counting backward just as if the stimulation had, no effect. However, when he tries to recall the object's name a few seconds later after the stimulation is turned off, he now has trouble remembering. Only stimulation at some points surrounding the language area has this dramatic effect of wiping out the memory of the sketch.
The language area just defined, by electrical stimulation during object naming, is one of the two language areas known from the studies of stroke patients. More than a century ago, the German neurologist Karl Wernicke described patients who talked nonsense but with good grammar, making up new words so as to talk in a jargon. A woman named Blanche, with damage to this area of her brain, when asked her name said, "Yes, it's not Mount Everest, Mont Blanc, blancmange, or almonds to put in water ... you know, you be clever and tell me." Such patients often fail to understand what others say to them, as well as talking nonsense themselves. They are inclined to talk excessively. These patients have strokes, I which destroy portions of left temporal and parietal lobes.
There is another language area in front of the motor strip, named after a French neurologist of the same era, Paul Broca. Destruction there causes a patient to speak with a telegraphic style of language, with all the little words missing and with little grammar. Talking about a movie, such a patient said, "Ah, policeman . . . ah . . . I know! . . . cashier! . . . money . . . ah! cigarettes . . . I know . . _. this . . . beer . . . mustache . . . " This patient understands what others say, knows he cannot talk correctly, and is frequently very frustrated by it. With more extensive damage, speech may be reduced to only a word or two, used over and over again for everything. Such was the situation in the patient under Broca's care in whom he first recognized this type of aphasia. Broca was on the staff of a large nursing home where this patient had lived for some years following a stroke. The patient's name was LeBorgne, but he was known to all as Tan-tan, for that is all he could say: "'Tan-tan . . . " At autopsy after Tan-tan died, Broca noted the damage to the left frontal lobe and related this to the language defect. This frontal language area is usually considered to be concerned with the output of language; the larger area of the parietal and temporal lobes is thought to be more concerned with the understanding of language. Thus the speech changes with the damage to the frontal area are often called "motor" or expressive" aphasia, while those after damage to parietal and temporal lobes are called "sensory" or "receptive" aphasia. ("Aphasia" literally means "no speech," but in practice the term is applied to someone with any kind of language defect after brain damage. Extensive damage to both frontal and parietal-temporal language areas, as in a large left hemisphere stroke, produces obvious deficits in both speech output and understanding, a combination called "global aphasia. " More subtle language disturbances have been described after small strokes damaging only part of one language area, or the connections between areas. Some patients with persisting damage to a small part of the parietal-temporal language area show difficulty only in coming up with the names of things, a condition known as "anomic aphasia." Such a patient, when shown a key, may say, "That's a, uh, I know that, it's, ah, a thing you put in a lock." Otherwise his speech is normal. Although anomic aphasics have difficulty only in naming, most other aphasic patients have naming difficulties as well as other speech deficits. Because such problems with naming impl objects are common to all types of aphasia, neurologists and neurosurgeons find this a useful test to be sure, that language is intact and to learn where the language area is located during operations such as Neil's. In another type of aphasia, spontaneous speech is usually present but there is a severe difficulty in repeating back spoken words. This deficit occurs with damage to a portion of the parietal-temporal language area, and is called "conduction aphasia."' The reverse of this, intact repetition but difficulty with initiating spontaneous speech, is occasionally seen after damage to the connections between the major language areas ("transcortical aphasia").
An even more unusual aphasia is an impaired ability to name colors. In these patients, the damage is on the inner side of the hemisphere, just below the area of cortex involved in vision. 6 Presumably this damage disconnects visual cortex from language cortex, which particularly affects color naming because colors are one of the few pure associations between naming and a visual input. There are few color clues from shape or usefulness; few other words help in identifying colors. Rarely is a patient completely mute. Stroke patients can usually produce a word or two, even with severe damage to language areas. Such patients may occasionally surprise their families by uttering a long string of invective: emotional speech is generally better preserved in severe motor aphasia, as is laughing and crying. We do not yet know the areas of the human brain which are important for emotional speech. In monkeys, the specific vocalizations produced by each species to attract mates or defend territory seem to be analogous to human emotional speech; in the monkey brain, these vocalizations depend upon the inner face of the hemisphere just in front of the foot area on the motor strip, a region called the supplementary motor area. 7 In man, damage to that area does temporarily render the patient mute; fortunately, essentially full recovery occurs in weeks. This area would be the logical candidate for human emotional speech. Emotional speech seems to be less lateralized to left brain than other language; indeed, some features of it, such as laughing, have been identified more often with right brain function. Despite their severe deficits in language, many aphasic patients are otherwise normal. Motor and sensory functions, hearing, and vision can be intact, and the patient may know that he does not speak correctly. When the problems of getting information into and out of the patient (by some mechanism other than speech) can be solved, tests often show normal ability to reason and make inferences. Brain damage leading to aphasia does not necessarily impair the nonlanguage aspects of complex thought. An aphasic artist may still draw, an aphasic musician may still compose. We do not know just how severely the language aspects of complex thought are impaired by this damage, largely because of the problem in testing such patients with impaired language. It has been argued that, with maturity, thoughts expressed in words are increasingly internalized into "inner speech." Young children tend to think out loud; adults keep those words to themselves. Such internalized phenomena are not easily studied, but it has been suggested that some types of aphasia severely impair this inner speech, especially aphasia after damage to Wernicke's area. In the preceding section we have presented the general pattern of language organization, with a frontal-lobe area for language output and a temporal-parietal area for language understanding. This pattern may be quite different in young children or left-handed persons, as'we shall discuss in a subsequent chapter. But even in the average right-handed adult, there seems to be considerable individual variation in the exact cortical location of language. For example, the sites where electrical stimulation of cortex alters naming are seldom exactly the same from one patient to the next. Only the rear one-third of the frontal language area, apparently necessary for the motor output of speech, seems to be relatively uniform between patients. In any other spot in the usual language areas, some patients will show naming changes indicating that they have language there, others will not. The individual pattern of language localization seems to be quite variable, perhaps as variable as our individual appearance. There are suggestions that overall verbal ability may correlate roughly with some patterns of language localization.
Surprisingly, two different languages spoken by the same patient may not use exactly the same areas of brain. Strokes damaging language areas in bilingual patients most commonly impair both languages equally or in proportion to how well they were spoken before the damage. The patient's native tongue, or the language in which he was most fluent, or the one used in his surroundings, is most likely to recover first. But an occasional case is a glaring exception. In these cases, the first and perhaps only language that recovers may be one that was not the native tongue, or the most fluent language, or the language of the present environment; rather, it is some other little-used language. Imagine the family's consternation when, after a stroke, Grandmother speaks only Croatian, which she spoke for a few years as an adolescent. And now no one else in the family speaks Croatian! These cases were especially perplexing to students of language until studies were done using electrical-stimulation mapping during naming in two languages. In bilingual patients, there are some cortical sites where naming is altered in only one language, as well as other sites where stimulation alters both languages. There seem to be brain areas used by only one language or the other, and presumably a stroke may destroy the area for one language (perhaps English) and leave the area for another intact (perhaps the area for Croatian). This does not necessarily mean that there are "first" and "second" language areas predetermined genetically. It may be that a large area of language cortex is needed to first learn any language. With continued use, smaller regions may suffice, freeing up other portions of language brain for new tasks, such as learning another language. Most aphasic patients have difficulty with reading and writing as well as speaking. Indeed, they tend to make the same kinds of mistakes in both spoken and written language. But occasionally brain damage will be followed by quite intact spoken language, but severe impairment 'of reading and/or writing. Impairment of only writing is quite rare, and usually associated with damage to wide areas of brain. But impairment of only reading is not uncommon. An occasional reading deficit follows left-frontal-lobe damage, above.the frontal language area. There the defect seems to be in tracking the printed words, as that area of brain is also involved in voluntary control of eye movements. But more commonly, isolated impairment of reading is due to damage to the back margin of the parietal-temporal (Wernicke) language area. Such damage is thought to disconnect the language area of the brain from visual input. 
Reading in languages that make use of pictographs, such as Chinese or the Kanji form of Japanese, seems to be less impaired by this type of brain damage (as is the recognition of certain italic-like types of script). Pictographs may be decoded in part by spatial mechanisms in the right brain, discussed in chapter 7. Aside from this, reading depends on the left side of the brain in most of us. The following patient illustrates this isolated reading disturbance after a stroke damaging the rear portions of parietal and temporal lobes. 
Fred had a bad headache, quite unlike any other he had ever had before. The next morning, he felt better and got dressed. He went downstairs and put breakfast on, then went out to get the newspaper. Upon sitting down to read it, he discovered to his astonishment that he could not read. He could see the paper, recognize the letters individually, but only the shortest two- and three-letter words made any sense. Later in the hospital, he was asked to write to dictation. He accurately wrote out in longhand an involved paragraph which was read aloud to him. Asked to read back what he had just written, he couldn't. Only the shortest words made any sense. He would try to piece together longer words but often made errors. His spoken language was normal. He had no blind spots in his visual fields, and his color vision was normal. A computerized tomographic scan showed that his stroke had damaged an area of the left parietal and temporal lobes, above and behind his left ear. This is to the rear of the language area but in front of the visual part of the brain, an area evidently more important for reading than for spoken language. A year later, Fred had recovered most of his ability to read. He tired easily, but could slowly read anything that he wanted (indeed, he read an early draft of this book). Whatever the function lost - reading, muscular control, language - at the time of the stroke, there is typically some recovery of function in the weeks and months which follow. But the extent of this recovery is quite variable. Sometimes, as in Fred's case, there is quite a lot of recovery. Sometimes, especially with more extensive damage, there is only a little recovery, although it may be six to twelve months or more before recovery reaches its limit. What happens in the brain during those weeks and months is not entirely clear. New neurons don't grow. Wounded neurons, however, return to duty. There may also be a reserve of neurons which can be pressed into action. It is unlikely to be a reserve of unused, spare neurons; a more likely analogy is the army reserve, whose members are called up out of many different occupations in time of need. Skills are widely spread around the population: just because someone specializes in banking does not mean that he or she cannot also function as a truck driver (but perhaps with somewhat less skill than a person who normally specialized in truck driving). Recovery of function thus probably reflects return of_ activity in damaged but not destroyed neurons and acquisition of secondary functions by other neurons. Indeed, with recovery after damage to language areas, there is now evidence that neurons on the other side of the brain have acquired such a secondary language function. |
 Continue to CHAPTER 4
Continue to CHAPTER 4
Notes and
References for this chapter Copyright ©1980 by |