|
Conversations with Neil’s Brain The Neural Nature of Thought & Language Copyright 1994 by William H. Calvin and George A. Ojemann. You may download this for personal reading but may not redistribute or archive without permission (exception: teachers should feel free to print out a chapter and photocopy it for students). William H. Calvin, Ph.D., is a neurophysiologist on the faculty of the Department of Psychiatry and Behavioral Sciences, University of Washington. George A. Ojemann, M.D., is a neurosurgeon and neurophysiologist on the faculty of the Department of Neurological Surgery, University of Washington. |
|
Deep in the Temporal Lobe, Just Across from the Brainstem This RealAudio file allows you to listen
to a sample of the audio monitor, amplifying the signal of several cortical neurons near the epileptic focus in an awake patient prior to removal of the epileptic region of brain.
IT’S QUIET IN THE O.R. during the second research study, the microelectrode recording.
The sequencing study went quickly, so we set up the apparatus that moved a microelectrode in
fine increments. Earlier we’d heard the crackle of neurons, their firing sounding like rain
on the roof. Irregular firing is par for the course in a cortical neuron, once you find one. But
finding one with a microelectrode is very much like fishing, and the fish aren’t biting right
now. |
|
IMMEDIATELY THE O.R. SEEMS to spring back to life. Now there is something for everyone
to do, rather than watching us fish. The circulating nurse appears with the fancy headgear,
carrying it atop a towel. Rather like, I reflect, a crown of jewels on a velvet cushion. The scrub nurse holds out a new pair of gloves for George. He slips them on over his other gloves. Then he takes the headgear from the circulating nurse and mounts it on his head, adjusting the headband himself. He swings down the little spotlight, making it point in the right direction. Next he swings down the little magnifiers, miniature binoculars a few inches long that stand outside his everyday eyeglasses. The binoculars are so skinny that he can look past them for ordinary maneuvering around the O.R. But when he looks straight ahead, he gets a magnified view of whatever is at arm’s length. The binoculars and the headlamp are for looking down deep, dark holes, and one is about to be created in Neil’s temporal lobe. Headgear adjustments complete, George strips off the now-contaminated gloves, leaving him with his original gloves still sterile. He takes a wet towel from the scrub nurse and wipes them off, just in case any glove powder was left behind. The circulating nurse takes the trailing fiber-optical cable from the spotlight and inserts it into the light source. A uniform spot of light suddenly appears on the sterile tent in front of George. 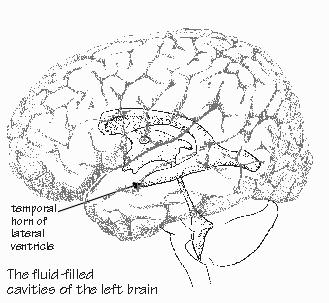 [FIGURE 76 The fluid-filled cavities of the brain] |
|
HALF AN HOUR LATER, the tip of Neil’s temporal lobe is gone. George whittled it
away, not with a knife, but very gently, using the tip of an ultrasonic vibrator. Any cells it
touches turn into a liquid, which is then sucked up along with any blood. This slow sculpturing
of the temporal lobe removes the tissue with preseizure activity on the earlier recordings, but
stops well short of the tags denoting the language and memory sites on the brain’s surface. As George worked down into the depths of Neil’s temporal lobe, he finally opened a hole into one of the brain’s natural cavities, the tip of the lateral ventricle, reservoir for cerebrospinal fluid. And some of the clear CSF flowed out. “Send for the EEG folks again,” George says. And I see the circulating nurse walk over to press the button on the memory phone that dials the beeper of the EEG staff, who are standing by in their offices. Or perhaps snacking in the hospital cafeteria. My stomach reminds me that lunchtime is long past. The scrub nurse, anticipating, places the little red box of strip electrodes on the front edge of her big tray so that George can reach them. The anesthesiologist reaches over to the infusion pump and, a receiving a confirming nod from George, turns it off so that Neil will start to wake up once again. George picks up a strip electrode. It is a flexible sheet of translucent material about the size of a paper clip, except that it also has a long pigtail of fine wire with a little plug on the end. There are four little silvery patches on one side of this sheet, that serve to monitor the voltages on the surface of the brain that they rest against. This strip electrode is going to be placed against an inner surface of the brain. That’s the inside surface of the lateral ventricle that is visible through the hole that George has created. Beneath that surface is the hippocampus, coordinator of memorizing. It is also the typical pacemaker for the types of seizures from which Neil suffers. Those round-the-clock recordings several weeks ago couldn’t be made from up close like this, only from the scalp. Here we have, literally, a window of opportunity through which to see whether the hippocampus is also participating in the early stages of Neil’s seizures. George tucks the little strip in through the window he has made. Close work — I can’t see a thing, myself. But George finally straightens back up and plugs the little wire into the cable leading back to the EEG machine in the gallery. I look back up to the gallery and, sure enough, the platoon of EEG people has arrived, and they are already examining the voltage tracings made by Neil’s hippocampus. The television monitor in the O.R. shows us exactly what they see. This electrical activity is quite different from what we saw this morning from the surface of the temporal lobe. There is much back-and-forth talk on the intercom about the little bursts of sharp positive-going wavelets, the hallmark of an epileptic process in the time in between seizures. They’re what are thought to occasionally drive the surrounding brain into seizure activity. Someone mentions that most seem to be coming from the far end of the strip electrode. And George immediately decides to move the strip electrode, to place it even further into the cavity so that it will rest against the hippocampus farther to the rear of the brain. We settle back to watch the EEG tracings once again. No doubt about it. Now the middle sites on the strip electrode are all showing the little positive wavelets. That means that this section of hippocampus (it’s a very long folded tubular structure running from front to back in the brain) ought to be removed — provided, of course, that this won’t cause more trouble than it cures. Another value judgment to be made. There is, fortunately, nearly a half century of experience with doing this kind of surgery, and many studies have been made of the patients afterward. Yes, if you run a lot of tests, there is some minor change in memory function. The more hippocampus that is removed, the more that memory is impaired. But patients don’t consider it a major problem. It’s not even a close call, given how much Neil’s seizures have increased in the last year. George announces that he’s going to take out the front part of hippocampus, as far back as the epileptic discharges are found, plus the uncus. Just as Portugal is the westernmost part of continental Europe, so the uncus is the part of temporal lobe that comes closest to the midline. And thus the brain stem. The uncus, alas, is a common cause of trouble. Neil still isn’t really awake yet, and hasn’t been heard from. But almost-awake is good enough, in this case. Many of Neil’s seizures occur as he is awakening, something that wasn’t realized until he was monitored around the clock. Now we’ve finally seen some pathophysiology that is likely close to the heart of the matter. The anesthesiologist starts the infusion pump again. 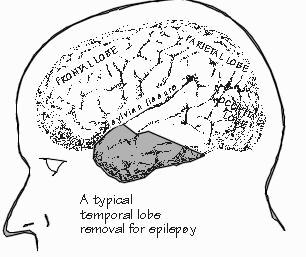 [FIGURE 77 Typical temporal lobe removal for epilepsy] |
|
GEORGE REMOVES SOME OF THE HIPPOCAMPUS as a block for the neuroanatomists to
study, and then goes to his gradual sculpturing to complete the removal. A bit further back, he stops again to remove a little crumb-sized piece of brain tissue intact, so that the pathologists can examine it. Using some forceps with little half cups on their tips, he pinches off a peninsula of tissue that he has left behind while sculpting. Usually it comes easily. Sometimes it doesn’t. “Label that as hippocampus,” he says to the scrub nurse as he hands her the forceps with the tissue still trapped inside. She drops the tissue into a little bottle that the circulating nurse holds out. “Felt soft,” he comments. In short, probably not scarred up — but the pathologist may see something more subtle. So now we’re all waiting to see what the tissue sample from the uncus will be like. George takes the cup forceps once again and begins maneuvering them down the hole. The uncus is a very short distance from the upper part of the brain stem, with only a fluid-filled gap in between. The uncus is rather like the spit of land that helps form the entrance to a harbor. And over on the other side of the gap is one of those lower-level centers of consciousness, to be carefully avoided. In between, there are a number of blood vessels. George is probably looking carefully, before closing the cup forceps around anything. George emerges again, forceps held closed around a piece of the uncus. About the time that he passes them to the scrub nurse, Neil’s head starts to shake back and forth. The anesthesiologist announces that Neil is having a seizure. But the shaking doesn’t resume, lasting less time than it took to comment on it. “It’s probably the uncus that started that seizure,” George says. “It felt tough when I pinched off a piece.” The original source of the seizures, at last? Cause and effect are all mixed up by now, of course. Even if there was once a single bit of anatomical pathology such as a scarred uncus, by now there are lots of well-trained followers that can cause trouble on their own. Which is why neurosurgeons remove whole regions of cerebral cortex, the hippocampus, and the amygdala. Removing small amounts of tissue simply does not get rid of the present problem — which is seizures, not scarring. No one wants to have to subject the patient to a second or third operation, removing more tissue each time, because too little was taken the first time. But it’s still nice to know where the trouble started, decades earlier. Looks as if it was the uncus, at least in Neil. And that’s a common pathological finding. Removing all that brain tissue, of course, also leaves a scar behind. But the surgery is designed to minimize it, just as plastic surgery replaces a large, ugly scar with a fine, hard-to-see scar. |
|
THE UNCUS IS PARTICULARLY prone to injury whenever the brain swells. Unlike the dura
elsewhere, the dura in this region is pulled taut — and it has an edge. It’s about the
closest thing to a sharp edge inside the skull, and nearby structures may rub across it when the
brain moves around inside the skull. There are three major routes by which the uncus seems to be damaged. All occur well before the onset of seizures. It seems that damage to the uncus is only the first step in the process that leads to epilepsy. 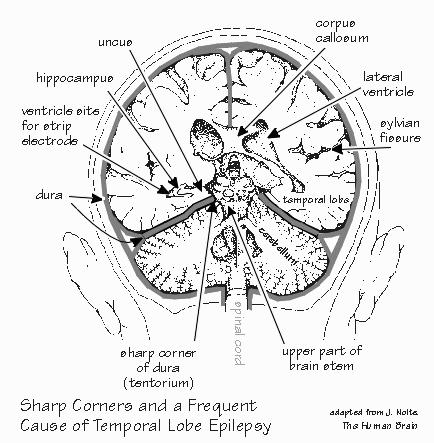 [FIGURE 78 How the inner surface of the temporal lobe is damaged] The infant’s head is somewhat compressed during birth, as it isn’t as rigid as it later becomes. If the head is a very tight fit in the birth canal, the brain may be squeezed somewhat, pushing it down toward the spinal cord. When that happens, the uncus is unusually vulnerable. It may be pushed into the brain stem while, at the same time, being bent around a sharp corner of dura. Such abrasion would indeed produce a scarred uncus, and sometimes a scarred hippocampus. Febrile seizures of early childhood, while the child is running a high fever, can do the same thing if the brain swells enough. But remember that most febrile seizures, like most childbirths, do no such thing — we’re talking about the extreme cases here. And head injuries can also cause trauma in this region because of that same edge of dura. The brain sits atop a narrow stalk of brain stem, rather like the head of a mushroom sits atop its stalk. You’d think that the brain couldn’t move, because of the skull. But it can be compressed. A sudden stop, as when the left side of the head encounters a car door frame, means that the right brain tries to compress the left brain. And so the brain moves atop the brain stem, potentially bruising the brain stem or the uncus. This edge of dura near the brain stem wasn’t exactly a good design. Neil’s weeks of memory problems following his accident suggests that his hippocampus was damaged (but it doesn’t seem to be scarred) or that its blood supply remained subnormal for a while. And that’s a real possibility. The arteries supplying the hippocampus run in the space between the uncus and the brain stem, right where they too could be traumatized. When blood vessels are traumatized, they usually shrink down and restrict the blood flow. |
|
BUT WHY SEIZURES, starting some time after the trauma to the uncus? Persisting seizures
usually don’t come on right after the damage, but rather months to years later, an average
of eight years after birth trauma or the febrile seizures of early life. We know which pieces of brain play a role in the genesis of the seizures because modern MRI scans show clearly the local damage, especially in the hippocampus. Yet we can only speculate on how all those pieces got involved. One presently popular theory is that there is a cascade of damage. Damaged neurons have the property of discharging in bursts of activity when they should produce only a single impulse. The neurons of the uncus have direct connections with the hippocampus. In the hippocampus are neurons with NMDA receptors - which, in response to bursts, tend to stay open a long time, letting calcium into the cell all the while. Too much internal calcium is toxic to neurons, and so the hippocampal neurons are secondarily damaged. They, in turn — so this theory goes — start to fire in bursts. This makes the perfectly normal neurons with which they are connected — often in the front part of the temporal lobe, including the outer surface — follow in that abnormal burst-firing pattern as well. When enough normal neurons repeatedly fire in synchronized bursts, that’s a focal seizure. The hippocampal damage — in this theory — is secondary to the original damage to the uncus. And when the hippocampal damage becomes extensive enough, seizures occur. There’s even some evidence that the attempts of the hippocampus to repair itself may make the whole situation worse, further increasing the chance for hippocampal neurons to fire in bursts. More subtle changes in the hippocampus following the long period of reduced blood supply might also compound the problem. Anticonvulsant drugs may work best on the followers, reducing the chances of things temporarily spreading even further to become a bigger seizure. Anticonvulsant drugs provide adequate seizure control for up to three-quarters of those with epilepsy; it is the remaining fourth that is evaluated for surgery. It’s likely that those patients whose seizures are not controlled by drugs represent a subpopulation with ongoing, progressive disease: that seizures beget seizures. These aren’t small subpopulations. Epilepsy is pretty common, about 0.5 to 1 percent of the population. That means the subpopulation with poorly controlled seizures on anticonvulsant drugs includes around 450,000 patients in the United States. New drugs for epilepsy are being continually evaluated — that’s a major research interest of Neil’s neurologist. And despite a cumbersome regulatory process, several new drugs for epilepsy have been approved. But these new drugs have, so far, produced only small reductions in the number of patients with poorly controlled seizures. Drugs and operations are really only “halfway” therapies for epilepsy, not unlike the iron lung stage of polio treatment. They address the symptoms, not the causes. What’s really needed is a better understanding of the causes, hopefully leading to prevention and a vast reduction in cost — as did the polio vaccine. That is what basic research is about. One prevention step is that people with head injuries are now usually treated with anticonvulsants — just as a precaution, hoping to avoid that cascade of damage following injury to the uncus. But a real understanding of seizure spread and calcium toxicity may someday prevent the secondary damage that leads to many kinds of epilepsy. |
|
NOW IT’S JUST A MATTER OF CLEANING UP and closing. How successful has
Neil’s operation been? Only time will tell for certain, but the more of the epileptic tissue
removed, the better the chances of seizure control. Neil’s final EEG recording, just before
closing, is “clean.” In an typical group of patients coming to an operation like Neil’s, around two-thirds will be free of seizures by the time the fourth and fifth postoperative years roll around. The patients with unusually localized temporal lobe disease have about an 80 percent chance of being seizure-free then. Patients with damage to both temporal lobes, but with seizures arising mostly from just one side, have only a 30 to 40 percent chance of being seizure-free — yet for the seizure-free group, it produces quite a change in their lives. They can get a driver’s license. If they were employed at the time of surgery, they are likely to have a better job a few years later. If they were students, they are more likely to become employed than those epileptics who continued uncontrolled without surgery. Evaluating patients for epilepsy surgery is complex, labor intensive, and expensive. So are the operations. That’s true of many “halfway” therapies: heart transplants, kidney dialysis, artificial hips, epilepsy operations. These advances in medical technology account for much of the rapid rise in health-care costs, a rise present in all developed countries, regardless of the “system” for health-care delivery. The health insurance companies are already reluctant to authorize these procedures or pay their full costs. Further limits on growth in health-care costs is likely to mean restricting the resources available for these technologies: limits on O.R.s, intensive-care beds, facilities for monitoring seizures, training of specialists who know how to handle these problems that are beyond the realm of family practice. All of this is likely to diminish the availability of these technologies and lead to longer waiting lists for them. Yet most figures indicate that the present level of epilepsy surgery takes care of only a fraction of the epileptics who need it. That number is estimated to be between 50,000 and 100,000 persons in the United States. The number of epilepsy operations done in the United States in any one year is well under 5,000. It is such resource-intensive procedures that could well be a major casualty of health-care reform. The real losers could be the patients like Neil who would benefit from them. |
|
SOMEHOW THE RESIDENT knows that it’s time to reappear. I saw her out at the sink
scrubbing again, and now she is getting gowned and gloved. We’d heard that she was busy in the O.R. next door, helping take care of a messy head injury from a head-on collision. Eventually she clears the obstacle course and joins us at Neil’s head. “We caught the guy just as he was starting to herniate,” the resident reports. I raise my eyebrows as the implications set in. She’s learned the art of understatement. You can’t translate this bit of vocabulary with the usual medical dictionary. The verb to herniate in the present tense is not found in most of them, which instead endlessly describe various fixed hernias, things bulging out here and there, in need of fixing sometime. It’s usually elective surgery. But every medical student knows what “He’s herniating” means. It refers to someone’s brain being seriously damaged over the course of a half hour, with fatal consequences ahead. It’s how people die from epidural hematomas, where bleeding from a leaking artery causes blood to pool outside the dura. Or from a burst aneurysm, somewhere inside the brain. The blood accumulates and pushes the brain down toward the brain stem. It’s one of the major medical emergencies that needs to be treated immediately. And it involves that same edge of dura that probably injured Neil’s brain. The temporal lobe gets pushed around the edge of the dura. That’s bad enough, in the long run. But it’s even worse in the short run, because that portion of temporal lobe gets pushed against the brain stem. The brain stem is apt to stop working when squeezed in this way. And so the patient is apt to stop breathing. While you can always put the patient on a respirator temporarily, all sorts of irreversible neurological damage gets done — unless you catch it very quickly by opening the skull and draining off the trapped blood. That’s evidently what she and the chief resident just did, the meaning of her simple words, “caught the guy.” Helping George finish up, after a few hours of that kind of action, is going to seem pretty tame to her. George has already finished with the final ultrasonic sculpturing around the biopsy sites, and has already gotten all of the bleeding under control. He takes her on a brief tour of the depths of the brain, pointing out where the scarred uncus was. And she’s very interested in that, as she didn’t get a chance to see it in her accident victim. It was what was threatening the brain stem, causing death to rapidly approach, but the surgery consisted of stopping the bleeding near the brain’s surface and relieving the pressure on the uncus. She and George are very busy for twenty minutes, stitching up the dura, all around the three edges of the flap. George summarizes what happened during the day as they both sew away, explaining the data we obtained and his rationale for his decisions about what to remove, especially how the results from the hippocampal strip electrode changed his mind. My view of Neil’s brain slowly disappears as they talk and sew. When they finish, the dura looks as taut as it normally does. If any bleeding starts outside the dura, it’ll have a hard time getting through that seam. She places some special sponges in the sites where rebleeding might occur — they are the kind that can be left behind and never removed — and then asks the scrub nurse for the drill. Time to start reattaching that big piece of Neil’s skull. She drills a little hole, no bigger than a pencil lead, near the edge of the skull opening. And another diagonally opposite. And a third and fourth, each near a corner of the bony window. George reaches across her to take the skull piece from its refuge atop the sterile tent where it has been resting for the last seven hours. He orients it to the opening, so that she can see where to drill the matching set of holes. While she does the drilling, standing off to one side, George threads four wires, very thin but very strong, through the first set of holes and bends them back into a hairpin shape. The resident holds the newly perforated skull piece up to the opening again. Everything matches. A quick look is taken around inside Neil’s skull. Everything’s stable. And so they string the wires through the new little holes in the skull cap, then seat it down into the beveled edges of the skull opening. A perfect fit. Some light is presumably still coming in through the saw cuts and the access holes in the corners, but it’s pretty much back to its customary darkness for Neil’s brain. The window is closing. The wires are twisted like a grocery tie, then the excess is snipped off. The next task is doing something about the five dime-sized holes that were drilled this morning to allow access for the saw. The scrub nurse has been mixing up some acrylic cement, beating it with a tongue depressor to get the desired stiffness. She scoops some up so that George can see it slowly drip back into the mixing bowl. Just the right consistency. The resident places some of the reabsorbable sponges in the bottom of each hole, to keep the acrylic off the dura. Then she takes the tongue depressor and begins filling the holes with the acrylic, smoothing off the surface with her gloved thumb, just as a carpenter fills nail holes before finishing. The acrylic will be solid in only a few minutes. But no acrylic is placed in the saw cuts. There is something better, when the gap is so narrow. The saw cuts will be filled in over the next few months as new bone grows into the gap. Eventually the skull will be structurally sound once more, the little wires no longer playing a role. Now it’s a matter of muscle. The big fanlike temporalis muscle, which helps run the left side of Neil’s jaw, is reconnected to the skull with another sewing job. Again the sutures are just to hold things in place while regrowth occurs. Then the skin flap is sewn up, though not as delicately as was the dura. The sterile tent is partially disassembled, and the rest of Neil comes into view. A sterile surgical dressing is wrapped around Neil’s head. Done.
|
 Conversations with Neil's Brain:
Conversations with Neil's Brain: The Neural Nature of Thought and Language (Addison-Wesley, 1994), co-authored with my neurosurgeon colleague, George Ojemann. It's a tour of the human cerebral cortex, conducted from the operating room, and has been on the New Scientist bestseller list of science books. It is suitable for biology and cognitive neuroscience supplementary reading lists. ISBN 0-201-48337-8. | AVAILABILITY widespread (softcover, US$12).
|